Current issue
Accepted manuscript
About the Journal
Scientific Council
Editorial Board
Regulatory and archival policy
Code of publishing ethics
Publisher
Information about the processing of personal data in relation to cookies and newsletter subscription
Archive
For Authors
For Reviewers
Contact
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Links
Sklep Wydawnictwa SUM
Biblioteka Główna SUM
Śląski Uniwersytet Medyczny w Katowicach
Privacy policy
Accessibility statement
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Familial angle-closure glaucoma in a 48-year-old female patient: A case report
1
Students’ Scientific Club at the Department of Ophthalmology, Faculty of Medical Sciences in Katowice, Medical University of Silesia, Katowice, Poland
2
Department of Ophthalmology, Faculty of Medical Sciences in Katowice, Medical University of Silesia, Katowice, Poland
3
Adult Ophthalmology Department, University Clinical Center named after Prof. K. Gibiński, Medical University of Silesia, Katowice, Poland
These authors had equal contribution to this work
Corresponding author
Wiktoria Żelazna
Studenckie Koło Naukowe, Klinika Okulistyki, Wydział Nauk Medycznych w Katowicach ŚUM, ul. Ceglana 35, 40-514 Katowice
Studenckie Koło Naukowe, Klinika Okulistyki, Wydział Nauk Medycznych w Katowicach ŚUM, ul. Ceglana 35, 40-514 Katowice
Ann. Acad. Med. Siles. 2026;80:195-202
KEYWORDS
TOPICS
ABSTRACT
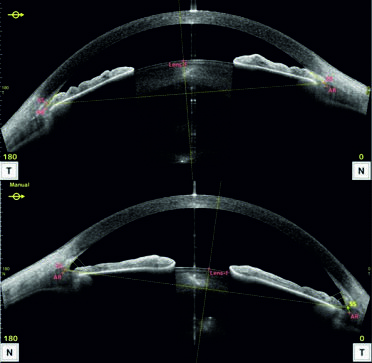
Primary angle-closure glaucoma (PACG) affects nearly 17 million people worldwide. A shallow anterior chamber and a short axial length increase the risk of angle closure and development of glaucomatous neuropathy. The progress of PACG is also associated with genetic predisposition. A 48-year-old female patient presented to the Outpatient Ophthalmology Clinic. Her sister had undergone two central decompressing vitrectomies due to advanced PACG. The patient was referred for additional examinations: tonometry, anterior segment optical coherence tomography (AS-OCT), gonioscopy, and static perimetry. The patient was qualified for prophylactic laser peripheral iridotomy (LPI) in both eyes. AS-OCT and gonioscopy revealed a closed angle in the right eye (oculus dexter – OD), a slit-like angle in the left eye (oculus sinister – OS), and a shallow anterior chamber in both eyes. The intraocular pressure (IOP) was measured at 20 mmHg in the OD and 15 mmHg in the OS. A peripheral relative visual field defect was found in the OD. Follow-up tonometry performed 14 months after the initial LPI showed an IOP of 27 mmHg in the OD. Timolol 0.5% was prescribed. Despite this, after 3 months, the IOP in the OD measured 22 mmHg. The patient was qualified for a repeat LPI in the OD. At follow-up, the IOP was 21 mmHg in the OD. Visual acuity was 1.0 in both eyes. LPI is the first-line treatment for PACG. Even though this procedure is highly effective, it does not guarantee long-term results. In case of recurrence, qualification for anti-glaucoma surgical intervention should be considered.
REFERENCES (26)
1.
Zhang N, Wang J, Chen B, Li Y, Jiang B. Prevalence of Primary Angle Closure Glaucoma in the Last 20 Years: A Meta-Analysis and Systematic Review. Front Med (Lausanne). 2021;7:624179. doi: 10.3389/fmed.2020.624179.
2.
European Glaucoma Society Terminology and Guidelines for Glaucoma, 5th Edition. Br J Ophthalmol. 2021;105(Suppl 1):1–169. doi: 10.1136/bjophthalmol-2021-egsguidelines.
3.
Weinreb RN, Aung T, Medeiros FA. The pathophysiology and treatment of glaucoma: a review. JAMA. 2014;311(18):1901–1911. doi: 10.1001/jama.2014.3192.
4.
Ahram DF, Alward WL, Kuehn MH. The genetic mechanisms of primary angle closure glaucoma. Eye (Lond). 2015;29(10):1251–1259. doi: 10.1038/eye.2015.124.
5.
Shah SN, Zhou S, Sanvicente C, Burkemper B, Apolo G, Li C, et al. Prevalence and Risk Factors of Blindness Among Primary Angle Closure Glaucoma Patients in the United States: An IRIS Registry Analysis. Am J Ophthalmol. 2024;259:131–140. doi: 10.1016/j.ajo.2023.11.007.
6.
Kondkar AA. Updates on Genes and Genetic Mechanisms Implicated in Primary Angle-Closure Glaucoma. Appl Clin Genet. 2021;14:89–112. doi: 10.2147/TACG.S274884.
7.
Wytyczne diagnostyki i leczenia jaskry (aktualizacja 2022). Polskie Towarzystwo Okulistyczne. Warszawa 2022.
8.
Lin Z, Liang Y, Wang N, Li S, Mou D, Fan S, et al. Peripheral anterior synechia reduce extent of angle widening after laser peripheral iridotomy in eyes with primary angle closure. J Glaucoma. 2013;22(5):374–379. doi: 10.1097/IJG.0b013e318241ba1d.
9.
Wright C, Tawfik MA, Waisbourd M, Katz LJ. Primary angle-closure glaucoma: an update. Acta Ophthalmol. 2016;94(3):217–225. doi: 10.1111/aos.12784.
10.
He M, Jiang Y, Huang S, Chang DS, Munoz B, Aung T, et al. Laser peripheral iridotomy for the prevention of angle closure: a single-centre, randomised controlled trial. Lancet. 2019;393(10181):1609–1618. doi: 10.1016/S0140-6736(18)32607-2.
11.
Bao YK, Xu BY, Friedman DS, Cho A, Foster PJ, Jiang Y, et al. Biometric Risk Factors for Angle Closure Progression After Laser Peripheral Iridotomy. JAMA Ophthalmol. 2023;141(6):516–524. doi: 10.1001/jamaophthalmol.2023.0937.
12.
Radhakrishnan S, Chen PP, Junk AK, Nouri-Mahdavi K, Chen TC. Laser Peripheral Iridotomy in Primary Angle Closure: A Report by the American Academy of Ophthalmology. Ophthalmology. 2018;125(7):1110–1120. doi: 10.1016/j.ophtha.2018.01.015.
13.
Azuara-Blanco A, Burr J, Ramsay C, Cooper D, Foster PJ, Friedman DS, et al. Effectiveness of early lens extraction for the treatment of primary angle-closure glaucoma (EAGLE): a randomised controlled trial. Lancet. 2016;388(10052):1389–1397. doi: 10.1016/S0140-6736(16)30956-4.
14.
Potop V, Corbu C. The role of clear lens extraction in angle closure glaucoma. Rom J Ophthalmol. 2017;61(4):244–248. doi: 10.22336/rjo.2017.44.
15.
Lundström M, Barry P, Henry Y, Rosen P, Stenevi U. Evidence-based guidelines for cataract surgery: guidelines based on data in the European Registry of Quality Outcomes for Cataract and Refractive Surgery database. J Cataract Refract Surg. 2012;38(6):1086–1093. doi: 10.1016/j.jcrs.2012.03.006.
16.
Chen PP, Lin SC, Junk AK, Radhakrishnan S, Singh K, Chen TC. The Effect of Phacoemulsification on Intraocular Pressure in Glaucoma Patients: A Report by the American Academy of Ophthalmology. Ophthalmology. 2015;122(7):1294–1307. doi: 10.1016/j.ophtha.2015.03.021.
17.
Singh K, Aggarwal H, Bhattacharyya M. Phacoemulsification in angle-closure glaucoma: A 360° evaluation. Indian J Ophthalmol. 2024;72(9):1275–1279. doi: 10.4103/IJO.IJO_1701_23.
18.
Kamińska A, Romaniak AM, Izdebska J, Szaflik JP. Surgical lens extraction with vitrectomy in patients with angle-closure glaucoma. Klinika Oczna/Acta Ophthalmologica Polonica. 2021;123(4):218–221. doi: 10.5114/ko.2021.111824.
19.
Noh HJ, Kim ST. Combined treatment of phacoemulsification and single-port limited pars plana vitrectomy in acute angle-closure glaucoma. Int J Ophthalmol. 2019;12(6):974–979. doi: 10.18240/ijo.2019.06.15.
20.
Sachdev R, Gupta A, Narula R, Deshmukh R. Limited vitrectomy in phacomorphic glaucoma. Indian J Ophthalmol. 2017;65(12):1422–1424. doi: 10.4103/ijo.IJO_668_17.
21.
Dada T, Kumar S, Gadia R, Aggarwal A, Gupta V, Sihota R. Sutureless single-port transconjunctival pars plana limited vitrectomy combined with phacoemulsification for management of phacomorphic glaucoma. J Cataract Refract Surg. 2007;33(6): 951–954. doi: 10.1016/j.jcrs.2006.12.037.
22.
Bayliss JM, Ng WS, Waugh N, Azuara-Blanco A. Laser peripheral iridoplasty for chronic angle closure. Cochrane Database Syst Rev. 2021;3(3):CD006746. doi: 10.1002/14651858.CD006746.pub4.
23.
Bourdon H, Aragno V, Baudouin C, Labbé A. Iridoplasty for plateau iris syndrome: a systematic review. BMJ Open Ophthalmol. 2019;4(1):e000340. doi: 10.1136/bmjophth-2019-000340.
24.
Yuasa Y, Sugimoto Y, Hirooka K, Ohkubo S, Higashide T, Sugiyama K, et al. Effectiveness of trabeculectomy with mitomycin C for glaucomatous eyes with low intraocular pressure on treatment eye drops. Acta Ophthalmol. 2020;98(1):e81–e87. doi: 10.1111/aos.14195.
25.
Ye W, Zhang S, Zhu S, Li J, Gu J, Zhao M, et al. 24-month prospective randomized comparison of ab externo penetrating canaloplasty versus trabeculectomy in primary angle-closure glaucoma. Asia Pac J Ophthalmol (Phila). 2025;14(3):100167. doi: 10.1016/j.apjo.2025.100167.
26.
Tham CC, Kwong YY, Baig N, Leung DY, Li FC, Lam DS. Phacoemulsification versus trabeculectomy in medically uncontrolled chronic angle-closure glaucoma without cataract. Ophthalmology. 2013;120(1):62–67. doi: 10.1016/j.ophtha.2012.07.021.
The Medical University of Silesia in Katowice, as the Operator of the annales.sum.edu.pl website, processes personal data collected when visiting the website. The function of obtaining information about Users and their behavior is carried out by voluntarily entered information in forms, saving cookies in end devices, as well as by collecting web server logs, which are in the possession of the website Operator. Data, including cookies, are used to provide services in accordance with the Privacy policy.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.