Current issue
Accepted manuscript
About the Journal
Scientific Council
Editorial Board
Regulatory and archival policy
Code of publishing ethics
Publisher
Information about the processing of personal data in relation to cookies and newsletter subscription
Archive
For Authors
For Reviewers
Contact
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Links
Sklep Wydawnictwa SUM
Biblioteka Główna SUM
Śląski Uniwersytet Medyczny w Katowicach
Privacy policy
Accessibility statement
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
The listeriosis brain abscess – the extremely rare complication during immunosuppressive therapy of autoimmune hepatitis
1
Department of Nephrology, Transplantation and Internal Medicine, Faculty of Medical Sciences in
Katowice, Medical University of Silesia, Katowice, Poland
2
Department of Gastroenterology and Hepatology, Faculty of Medical Sciences in Katowice,
Medical University of Silesia, Katowice, Poland
Corresponding author
Joanna Musialik
Katedra i Klinika Gastroenterologii i Hepatologii, ul. Medyków 14, 40-752 Katowice, Uniwersyteckie Centrum Kliniczne im. prof. K. Gibińskiego ŚUM
Katedra i Klinika Gastroenterologii i Hepatologii, ul. Medyków 14, 40-752 Katowice, Uniwersyteckie Centrum Kliniczne im. prof. K. Gibińskiego ŚUM
KEYWORDS
TOPICS
ABSTRACT
In recent years, there has been a steady increase in the number of people receiving immunosuppressive treatment. The ongoing development of these therapies, although effective in controlling autoimmune disease, brings with it new diagnostic and therapeutic challenges due to complex modulation of cellular and humoral responses. Despite significant therapeutic benefits, their use is associated with the risk of developing opportunistic infections, which are almost unrecognised in immunocompetent persons. We present a case of neuroinfection caused by Listeria monocytogenes complicated by brain abscess in an autoimmune hepatitis female patient treated with prednisone and mercaptopurine. Importantly, the disease initially presented with non-specific neurological symptoms, which might have delayed diagnosis. Nevertheless, an early lumbar puncture, cerebrospinal fluid testing with identification of the most common pathogens, and imaging tests allowed for diagnosis and implementation of appropriate antibiotic therapy, which resulted in the expected clinical improvement. This case highlights that patients receiving immunosuppressive therapy may develop serious opportunistic infections, and early diagnosis and implementation of right treatment are crucial for improving prognosis and minimising complications.
ACKNOWLEDGEMENTS
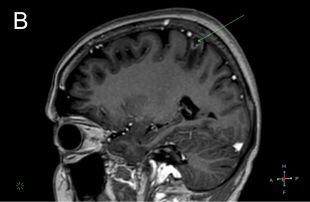
Acknowledgements: We would like to thank Dr Anna Kwaśniewska, MD, PhD for her help in magnetic resonance scans analysis and prepare for publication.
REFERENCES (17)
1.
Giles AJ, Hutchinson MND, Sonnemann HM, Jung J, Fecci PE, Ratnam NM, et al. Dexamethasone-induced immunosuppression: mechanisms and implications for immunotherapy. J Immunother Cancer. 2018;6(1):51. doi: 10.1186/s40425-018-0371-5.
2.
Orlicka K, Barnes E, Culver EL. Prevention of infection caused by immunosuppressive drugs in gastroenterology. Ther Adv Chronic Dis. 2013;4(4):167–185. doi: 10.1177/2040622313485275.
3.
Manns MP, Vogel A. Autoimmune hepatitis, from mechanisms to therapy. Hepatology. 2006;43(2 Suppl 1):132–144. doi: 10.1002/hep.21059.
4.
Czaja AJ, Freese DK; American Association for the Study of Liver Disease. Diagnosis and treatment of autoimmune hepatitis. Hepatology. 2002;36(2):479–497. doi: 10.1053/jhep.2002.34944.
5.
Yassin W, Nasser R, Veitsman E, Saadi T. The Effectiveness of Measuring Thiopurine Metabolites in the Treatment of Autoimmune Hepatitis Patients. Turk J Gastroenterol. 2024;35(3):232–238. doi: 10.5152/tjg.2024.22838.
6.
Cutolo M, Seriolo B, Pizzorni C, Secchi ME, Soldano S, Paolino S, et al. Use of glucocorticoids and risk of infections. Autoimmun Rev. 2008;8(2):153–155. doi: 10.1016/j.autrev.2008.07.010.
7.
Naganuma M, Kunisaki R, Yoshimura N, Takeuchi Y, Watanabe M. A prospective analysis of the incidence of and risk factors for opportunistic infections in patients with inflammatory bowel disease. J Gastroenterol. 2013;48(5):595–600. doi: 10.1007/s00535-012-0686-9.
8.
Lübbert C, Johann C, Kekulé AS, Worlitzsch D, Weis S, Mössner J, et al. Immunosuppressive treatment as a risk factor for the occurrence of clostridium difficile infection (CDI). [Article in German]. Z Gastroenterol. 2013;51(11):1251–1258. doi: 10.1055/s-0033-1335505.
9.
Wałecka-Zacharska E, Bania J. Listeria monocytogenes – patogen, który wie, jak przetrwać. Życie Wet. 2014;89(11):917–919.
10.
Godziszewska S, Musioł E, Duda I. Listeriosis – a dangerous, contagious disease. Meningitis caused by Listeria monocytogenes – case report. [Article in Polish]. Ann Acad Med Siles. 2015;69:118–124. doi: 10.18794/aams/33100.
11.
Vasconcelos M, Moreira AP, Pereira CS, Duarte Armindo R, Noronha C. Brain Abscess Caused by Listeria monocytogenes: A Rare Case of Supratentorial Neurolisteriosis. Cureus. 2024;16(2):e54521. doi: 10.7759/cureus.54521.
12.
Qu H, Wang Y, Diao H, Ren G, Wang Z, Shang J, et al. Clinical characteristics of 15 patients with Listeria meningitis in adult. Heliyon. 2023;10(1):e23755. doi: 10.1016/j.heliyon.2023.e23755.
13.
Disson O, Lecuit M. Targeting of the central nervous system by Listeria monocytogenes. Virulence. 2012;3(2):213–221. doi: 10.4161/viru.19586.
14.
Zhang J, Huang S, Xu L, Tao M, Zhao Y, Liang Z. Brain abscess due to listeria monocytogenes: A case report and literature review. Medicine. 2021;100(31):e26839. doi: 10.1097/MD.0000000000026839.
15.
Bristowe H, Dissanayake K, Chandra J, Arias M. Listeria brain abscess: a therapeutically challenging rare presentation of listeriosis. BMC Infect Dis. 2024;24(1):477. doi: 10.1186/s12879-024-09295-z.
16.
Trachuk P, Marin Saquicela T, Levi M, Khedimi R. Listeria brain abscess in a patient with autoimmune hepatitis. IDCases. 2019;17:e00569. doi: 10.1016/j.idcr.2019.e00569.
17.
Ezquerra A, Martínez B, García-Buey L. Invasive listeriosis in a patient with autoimmune hepatitis on glucocorticosteroid therapy. Med Clin. 2022;158(1):39. doi: 10.1016/j.medcli.2021.03.015.
The Medical University of Silesia in Katowice, as the Operator of the annales.sum.edu.pl website, processes personal data collected when visiting the website. The function of obtaining information about Users and their behavior is carried out by voluntarily entered information in forms, saving cookies in end devices, as well as by collecting web server logs, which are in the possession of the website Operator. Data, including cookies, are used to provide services in accordance with the Privacy policy.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.