Current issue
Accepted manuscript
About the Journal
Scientific Council
Editorial Board
Regulatory and archival policy
Code of publishing ethics
Publisher
Information about the processing of personal data in relation to cookies and newsletter subscription
Archive
For Authors
For Reviewers
Contact
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Links
Sklep Wydawnictwa SUM
Biblioteka Główna SUM
Śląski Uniwersytet Medyczny w Katowicach
Privacy policy
Accessibility statement
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Transforaminal lumbar interbody fusion L4/L5 in a 72-year-old Jehovah’s Witness with a history of prostate cancer: A case report following patient blood management standards
1
Department of Medical Biophysics, Faculty of Medical Sciences in Katowice, Medical University of Silesia, Katowice, Poland
2
Gabriel Narutowicz Municipal Specialist Hospital, Cracow, Poland
Corresponding author
Ann. Acad. Med. Siles. 2026;80:171-178
KEYWORDS
lumbar spinal stenosisdiscectomytransforaminal lumbar interbody fusionpatient blood managementneurogenic claudicationspine surgery
TOPICS
ABSTRACT
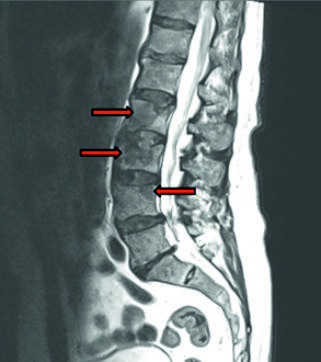
Lumbar spinal stenosis (LSS) is a common degenerative condition in older adults, leading to chronic low back pain, neurogenic claudication, reduced functional capacity, and impaired quality of life. It most frequently affects the L4/L5 and L5/S1 levels. Surgical intervention improves patient outcomes when conservative treatment fails. Coexisting conditions, such as prostate cancer with spinal metastases, increase the risk of fractures and bleeding. Refusal of blood transfusions by Jehovah’s Witnesses requires comprehensive patient blood management (PBM), including preoperative optimization, meticulous intraoperative hemostasis, and postoperative support. A 72-year-old man with chronic low back pain, neurogenic claudication, and progressive neurological deficits, with a history of prostate cancer and complete refusal of blood transfusions, presented for treatment. Magnetic resonance imaging (MRI) revealed critical stenosis at L4/L5 and degenerative changes at L2–L4. Conservative therapy was ineffective. The patient underwent transforaminal lumbar interbody fusion (TLIF) with pedicle screw fixation and a biopsy of L3. Recovery was uneventful, neurological deficits resolved, and follow-up MRI confirmed adequate decompression of neural structures. Histopathology demonstrated prostate cancer metastases. The procedure provided decompression and spinal
stabilization while minimizing blood loss through PBM measures, including optimization of erythropoiesis, tranexamic acid administration, precise hemostasis, and monitoring of hidden blood loss. TLIF with PBM is safe and effective in older patients with severe lumbar stenosis, coexisting malignancy, and transfusion restrictions. Multidisciplinary planning and meticulous surgical technique support neurological recovery and allow continuation of oncological treatment.
REFERENCES (40)
1.
Lafian AM, Torralba KD. Lumbar Spinal Stenosis in Older Adults. Rheum Dis Clin North Am. 2018;44(3):501–512. doi: 10.1016/j.rdc.2018.03.008.
2.
Malik KN, Giberson C, Ballard M, Camp N, Chan J. Pain Management Interventions in Lumbar Spinal Stenosis: A Literature Review. Cureus. 2023;15(8):e44116. doi: 10.7759/cureus.44116.
3.
Katz JN, Harris MB. Clinical practice: Lumbar spinal stenosis. N Engl J Med. 2008;358(8):818–825. doi: 10.1056/NEJMcp0708097.
4.
Ishimoto Y, Yoshimura N, Muraki S, Yamada H, Nagata K, Hashizume H, et al. Associations between radiographic lumbar spinal stenosis and clinical symptoms in the general population: the Wakayama Spine Study. Osteoarthritis Cartilage. 2013;21(6):783–788. doi: 10.1016/j.joca.2013.02.656.
5.
Kalichman L, Cole R, Kim DH, Li L, Suri P, Guermazi A, et al. Spinal stenosis prevalence and association with symptoms: the Framingham Study. Spine J. 2009;9(7):545–550. doi: 10.1016/j.spinee.2009.03.005.
6.
Katz JN, Zimmerman ZE, Mass H, Makhni MC. Diagnosis and Management of Lumbar Spinal Stenosis: A Review. JAMA. 2022;327(17):1688–1699. doi: 10.1001/jama.2022.5921.
7.
Meng B, Bunch J, Burton D, Wang J. Lumbar interbody fusion: recent advances in surgical techniques and bone healing strategies. Eur Spine J. 2021;30(1):22–33. doi: 10.1007/s00586-020-06596-0.
8.
Potter BK, Freedman BA, Verwiebe EG, Hall JM, Polly DW Jr, Kuklo TR. Transforaminal lumbar interbody fusion: clinical and radiographic results and complications in 100 consecutive patients. J Spinal Disord Tech. 2005;18(4):337–346. doi: 10.1097/01.bsd.0000166642.69189.45.
9.
Hey HW, Hee HT. Lumbar degenerative spinal deformity: Surgical options of PLIF, TLIF and MI-TLIF. Indian J Orthop. 2010;44(2):159–162. doi: 10.4103/0019-5413.62066.
10.
Bubendorf L, Schöpfer A, Wagner U, Sauter G, Moch H, Willi N, et al. Metastatic patterns of prostate cancer: An autopsy study of 1,589 patients. Hum Pathol. 2000;31(5):578–583. doi: 10.1053/hp.2000.6698.
11.
Coleman R, Hadji P, Body JJ, Santini D, Chow E, Terpos E, et al. Bone health in cancer: ESMO Clinical Practice Guidelines. Ann Oncol. 2020;31(12):1650–1663. doi: 10.1016/j.annonc.2020.07.019.
12.
Baldessari C, Pipitone S, Molinaro E, Cerma K, Fanelli M, Nasso C, et al. Bone Metastases and Health in Prostate Cancer: From Pathophysiology to Clinical Implications. Cancers. 2023;15(5):1518. doi: 10.3390/cancers15051518.
13.
Radek A, Zapałowicz K, Maciejczak A, Karbownik J, Radek M, Gasiń-ski P, et al. Strategy in the diagnostics and therapy of tumours of the spine. Ortop Traumatol Rehabil. 2003;5(4):530–533.
14.
Sacks DA, Koppes RH. Blood transfusion and Jehovah’s Witnesses: medical and legal issues in obstetrics and gynecology. Am J Obstet Gynecol. 1986;154(3):483–486. doi: 10.1016/0002-9378(86)90586-7.
15.
Wujtewicz M. Perioperative strategies in patients who refuse blood product transfusion. Pol Przegl Chir. 2020;92(5):1–5. doi: 10.5604/01.3001.0014.1508.
16.
Gohel MS, Bulbulia RA, Slim FJ, Poskitt KR, Whyman MR. How to approach major surgery where patients refuse blood transfusion (including Jehovah’s Witnesses). Ann R Coll Surg Engl. 2005;87(1):3–14. doi: 10.1308/1478708051414.
17.
Weinstein JN, Tosteson TD, Lurie JD, Tosteson ANA, Blood E, Hanscom B, et al. Surgical versus nonsurgical therapy for lumbar spinal stenosis. N Engl J Med. 2008;358(8):794–810. doi: 10.1056/NEJMoa0707136.
18.
Planty-Bonjour A, Kerdiles G, François P, Destrieux C, Velut S, Zemmoura I, et al. Cauda Equina Syndrome: Poor Recovery Prognosis Despite Early Treatment. Spine. 2022;47(2):105–113. doi: 10.1097/BRS.0000000000004170.
19.
Li W, Wei H, Zhang R. Different lumbar fusion techniques for lumbar spinal stenosis: a Bayesian network meta-analysis. BMC Surg. 2023;23(1):345. doi: 10.1186/s12893-023-02242-w.
20.
Gum JL, Reddy D, Glassman S. Transforaminal Lumbar Interbody Fusion (TLIF). JBJS Essent Surg Tech. 2016;6(2):e22. doi: 10.2106/JBJS.ST.15.00003.
21.
Hafez AA, Ashry AH, Elsayed A, Tayeb AE, ElShenawy MBAS. Incidence of Iatrogenic Lumbar Spinal Instability after Laminectomy, Discectomy or Facetectomy. Open Access Maced J Med Sci. 2021;9(B):588–592. doi: 10.3889/oamjms.2021.6256.
22.
Spina NT, Moreno GS, Brodke DS, Finley SM, Ellis BJ. Biomechanical effects of laminectomies in the human lumbar spine: a finite element study. Spine J. 2021;21(1):150–159. doi: 10.1016/j.spinee.2020.07.016.
23.
Pradeep K, Pal B, Mukherjee K, Shetty GM. Transforaminal lumbar interbody fusion (TLIF) surgery: A finite element analysis of open and minimally invasive approach on L4-L5 segment. Heliyon. 2025;11(2):e41842. doi: 10.1016/j.heliyon.2025.e41842.
24.
Ke W, Zhang T, Wang B, Hua W, Wang K, Cheung JPY, et al. Biomechanical Comparison of Different Surgical Approaches for the Treatment of Adjacent Segment Diseases after Primary Transforaminal Lumbar Interbody Fusion: A Finite Element Analysis. Orthop Surg. 2023;15(10):2701–2708. doi: 10.1111/os.13866.
25.
de Kunder SL, van Kuijk SMJ, Rijkers K, Caelers IJMH, van Hemert WLW, de Bie RA, et al. Transforaminal lumbar interbody fusion (TLIF) versus posterior lumbar interbody fusion (PLIF) in lumbar spondylolisthesis: a systematic review and meta-analysis. The Spine Journal. 2017 Jun 22;17(11):1712–1721. doi: 10.1016/j.spinee.2017.06.018.
26.
Levin JM, Tanenbaum JE, Steinmetz MP, Mroz TE, Overley SC. Posterolateral fusion (PLF) versus transforaminal lumbar interbody fusion (TLIF) for spondylolisthesis: a systematic review and meta-analysis. Spine J. 2018;18(6):1088–1098. doi: 10.1016/j.spinee.2018.01.028.
27.
Kang T, Park SY, Nam JJ, Lee SH, Park JH, Suh SW. Patient Blood Management During Lumbar Spinal Fusion Surgery. World Neurosurg. 2019;130:e566–e572. doi: 10.1016/j.wneu.2019.06.153.
28.
Yildiz Y, Motov S, Stengel F, Bertulli L, Fischer G, Bättig L, et al. Influence of Frailty on Clinical and Radiological Outcomes in Patients Undergoing Transforaminal Lumbar Interbody Fusion—Analysis of a Controlled Cohort of 408 Patients. J Clin Med. 2025;14(6):1814. doi: 10.3390/jcm14061814.
29.
Yang Y, Zhang L, Liu B, Pang M, Xie P, Chen Z, et al. Hidden and overall haemorrhage following minimally invasive and open transforaminal lumbar interbody fusion. J Orthop Traumatol. 2017;18(4):395–400. doi: 10.1007/s10195-017-0464-9.
30.
Xiao K, Zhuo X, Peng X, Wu Z, Li B. The efficacy and safety of tranexamic acid in lumbar surgery: A meta-analysis of randomized-controlled trials. Jt Dis Relat Surg. 2022;33(1):57–85. doi: 10.52312/jdrs.2022.432.
31.
Lei F, Li Z, He W, Tian X, Zheng L, Kang J, et al. Hidden blood loss and the risk factors after posterior lumbar fusion surgery: A retrospective study. Medicine. 2020;99(19):e20103. doi: 10.1097/MD.0000000000020103.
32.
Phan K, Rao PJ, Kam AC, Mobbs RJ. Minimally invasive versus open transforaminal lumbar interbody fusion for treatment of degenerative lumbar disease: systematic review and meta-analysis. Eur Spine J. 2015;24(5):1017–1030. doi: 10.1007/s00586-015-3903-4.
33.
Nishizawa M, Glassman SD, Djurasovic M, Crawford CH 3rd, Gum JL, Dimar JR 2nd, et al. Discharge Hemoglobin Impacts Functional Recovery After Lumbar Fusion. Spine. 2025; doi: 10.1097/BRS.0000000000005440. Online ahead of print.
34.
Briguglio M, Perazzo P, Langella F, Crespi T, De Vecchi E, Riso P, et al. Prediction of Long-Term Recovery From Disability Using Hemoglobin-Based Models: Results From a Cohort of 1,392 Patients Undergoing Spine Surgery. Front Surg. 2022;9:850342. doi: 10.3389/fsurg.2022.850342.
35.
Godlewski B. Assessing quality of life in spinal surgery. Anesth Pain Med. 2012;1(4):275–276. doi: 10.5812/aapm.3552.
36.
Zhao Y, Huang Y, Wang Z, Song Y, Chen Q, Feng G. Geriatric nutrition risk index is useful to assess the risk of postoperative urinary retention in elderly patient undergoing lumber interbody fusion. Eur Spine J. 2025;34(9):4057–4063. doi: 10.1007/s00586-025-08957-z.
37.
Poeppel TD, Handkiewicz-Junak D, Andreeff M, Becherer A, Bockisch A, Fricke E, et al. EANM guideline for radionuclide therapy with radium-223 of metastatic castration-resistant prostate cancer. Eur J Nucl Med Mol Imaging. 2018;45(5):824–845. doi: 10.1007/s00259-017-3900-4.
38.
Van Nieuwenhove S, Van Damme J, Padhani AR, Vandecaveye V, Tombal B, Wuts J, et al. Whole‐body magnetic resonance imaging for prostate cancer assessment: Current status and future directions. J Magn Reson Imaging. 2022;55(3):653–680. doi: 10.1002/jmri.27485.
39.
Lin CH, Wu YJ, Chang CW, Tam KW, Loh EW. Unilateral versus bilateral pedicle screw fixation in minimally invasive transforaminal lumbar interbody fusion: a systematic review and meta-analysis of randomized controlled trials. Arch Orthop Trauma Surg. 2025;145(1):148. doi: 10.1007/s00402-024-05749-w.
40.
Arana E, Kovacs FM, Royuela A, Asenjo B, Pérez-Ramírez Ú, Zamora J, et al. Spine Instability Neoplastic Score: agreement across different medical and surgical specialties. Spine J. 2016;16(5):591–599. doi: 10.1016/j.spinee.2015.10.006.
The Medical University of Silesia in Katowice, as the Operator of the annales.sum.edu.pl website, processes personal data collected when visiting the website. The function of obtaining information about Users and their behavior is carried out by voluntarily entered information in forms, saving cookies in end devices, as well as by collecting web server logs, which are in the possession of the website Operator. Data, including cookies, are used to provide services in accordance with the Privacy policy.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.