Current issue
Accepted manuscript
About the Journal
Scientific Council
Editorial Board
Regulatory and archival policy
Code of publishing ethics
Publisher
Information about the processing of personal data in relation to cookies and newsletter subscription
Archive
For Authors
For Reviewers
Contact
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Links
Sklep Wydawnictwa SUM
Biblioteka Główna SUM
Śląski Uniwersytet Medyczny w Katowicach
Privacy policy
Accessibility statement
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Determinants of breast cancer prevention in a group of women with cancer suspicion
1
Państwowa Akademia Nauk Stosowanych w Krośnie / State University of Applied Sciences in Krosno, Poland
Corresponding author
Joanna Grzesik-Gąsior
Państwowa Akademia Nauk Stosowanych w Krośnie, ul. Kazimierza Wielkiego 6, 38-400 Krosno
Państwowa Akademia Nauk Stosowanych w Krośnie, ul. Kazimierza Wielkiego 6, 38-400 Krosno
Ann. Acad. Med. Siles. 2024;78:73-81
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Due to constant increase incidence of breast cancer in the world, the most important aspect is monitoring of preventive actions and increasing the health awareness of breast cancer in societies, especially in the group of people with high probability of oncological problems. The aim of the study was to analyze selected factors determining women’s uptake of breast cancer prevention activities.
Material and methods:
The study was conducted by diagnostic survey among 121 women, patients of the oncology clinic in Brzozów. Women’s knowledge, sociodemographic indicators and positive family history of breast cancer were assessed. Research tool was the proprietary questionnaire. The chi-square (χ2) test was used to verify the hypotheses. A significance level of p < 0.05 was assumed.
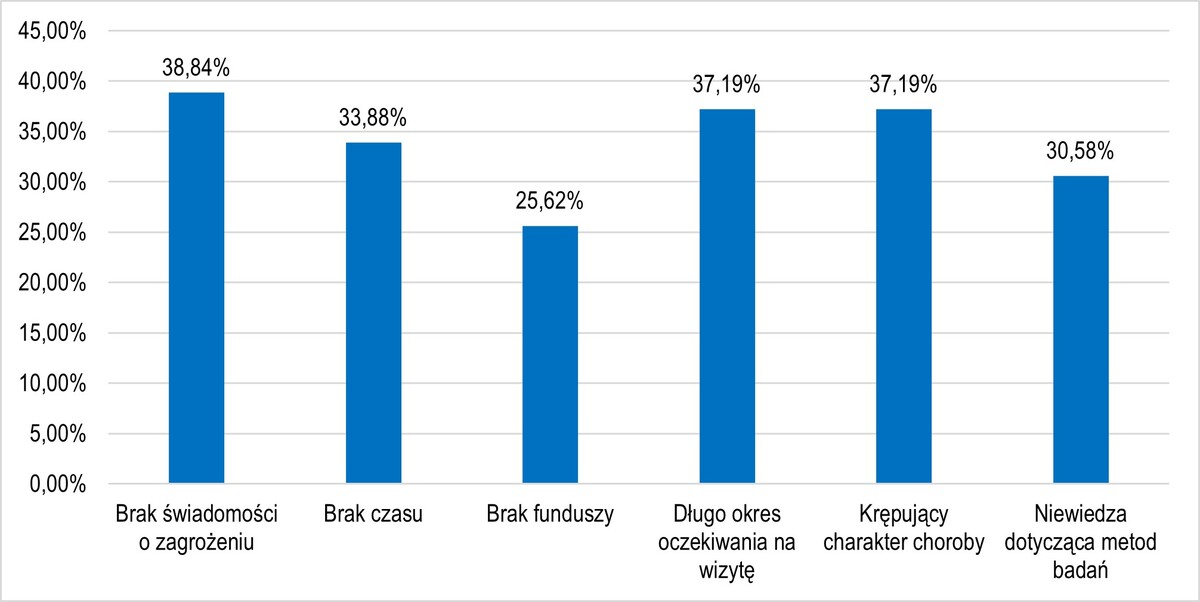
Results:
The most common source of knowledge about breast cancer prevention was the Internet (52.89%), and the main reason for forgoing preventive examinations was lack of awareness of the disease’s risks (38.84%). Over 30% of the respondents had a low level of knowledge which was statistically diverse in terms of education (p < 0.001) and respondents age (p = 0.01). Younger and better educated women have a higher level of knowledge, which was related to the regularity of preventive actions (p = 0.048) and breast self-examination (p < 0.001). The occurrence of breast cancer in the family was impact to regulary self-examination and diagnostic tests (p < 0.001).
Conclusions:
The level of knowledge in the term of breast cancer prevention wasn’t satisfactory and need supplementing. The most frequently indicated source of information was Internet what show need to increase the participation of medical specialists in oncology education. The most important predictors of taking regularly preventive actions were young age, higher level of knowledge, higher education and a positive family history (breast cancer).
Due to constant increase incidence of breast cancer in the world, the most important aspect is monitoring of preventive actions and increasing the health awareness of breast cancer in societies, especially in the group of people with high probability of oncological problems. The aim of the study was to analyze selected factors determining women’s uptake of breast cancer prevention activities.
Material and methods:
The study was conducted by diagnostic survey among 121 women, patients of the oncology clinic in Brzozów. Women’s knowledge, sociodemographic indicators and positive family history of breast cancer were assessed. Research tool was the proprietary questionnaire. The chi-square (χ2) test was used to verify the hypotheses. A significance level of p < 0.05 was assumed.
Results:
The most common source of knowledge about breast cancer prevention was the Internet (52.89%), and the main reason for forgoing preventive examinations was lack of awareness of the disease’s risks (38.84%). Over 30% of the respondents had a low level of knowledge which was statistically diverse in terms of education (p < 0.001) and respondents age (p = 0.01). Younger and better educated women have a higher level of knowledge, which was related to the regularity of preventive actions (p = 0.048) and breast self-examination (p < 0.001). The occurrence of breast cancer in the family was impact to regulary self-examination and diagnostic tests (p < 0.001).
Conclusions:
The level of knowledge in the term of breast cancer prevention wasn’t satisfactory and need supplementing. The most frequently indicated source of information was Internet what show need to increase the participation of medical specialists in oncology education. The most important predictors of taking regularly preventive actions were young age, higher level of knowledge, higher education and a positive family history (breast cancer).
FUNDING
No financial support was received.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
REFERENCES (22)
1.
Global breast cancer initiative implementation framework: assessing, strengthening and scaling up of services for the early detection and management of breast cancer. Executive summary [pdf]. World Health Organization. Geneva 2023. Licencja: CC BY-NC-SA 3.0 IGO. Dostępny w internecie: https://iris.who.int/bitstream... [dostęp: 08.03.2024].
2.
Europejski System Informacji o Raku – ECIS [online] https://ecis.jrc.ec.europa.eu [dostęp: 08.03.2024].
3.
Britt K.L., Cuzick J., Phillips K.A. Key steps for effective breast cancer prevention. Nat. Rev. Cancer 2020; 20(8): 417–436, doi: 10.1038/s41568-020-0266-x.
4.
Kolak A., Kamińska M., Sygit K., Budny A., Surdyka D., Kukiełka-Budny B. i wsp. Primary and secondary prevention of breast cancer. Ann. Agric. Environ. Med. 2017; 24(4): 549–553, doi: 10.26444/aaem/75943.
5.
Hunt K.K., Euhus D.M., Boughey J.C., Chagpar A.B., Feldman S.M., Hansen N.M. i wsp. Society of Surgical Oncology Breast Disease Working Group statement on prophylactic (risk-reducing) mastectomy. Ann. Surg. Oncol. 2017; 24(2): 375–397, doi: 10.1245/s10434-016-5688-z.
6.
Thorat M.A., Balasubramanian R. Breast cancer prevention in high-risk women. Best Pract. Res. Clin. Obstet. Gynaecol. 2020; 65: 18–31, doi: 10.1016/j.bpobgyn.2019.11.006.
7.
Kashyap D., Pal D., Sharma R., Garg V.K., Goel N., Koundal D. i wsp. Global increase in breast cancer incidence: risk factors and preventive measures. Biomed. Res. Int. 2022; 2022: 9605439, doi: 10.1155/2022/9605439.
8.
Harkness E.F., Astley S.M., Evans D.G. Risk-based breast cancer screening strategies in women. Best Pract. Res. Clin. Obstet. Gynaecol. 2020; 65: 3–17, doi: 10.1016/j.bpobgyn.2019.11.005.
9.
Jafari S.H., Saadatpour Z., Salmaninejad A., Momeni F., Mokhtari M., Nahand J.S. i wsp. Breast cancer diagnosis: Imaging techniques and biochemical markers. J. Cell. Physiol. 2018; 233(7): 5200–5213, doi: 10.1002/jcp.26379.
10.
Harris M., Taylor G. Statystyka medyczna: jasno i zrozumiale. Makmed. Lublin 2021.
11.
Dydjow-Bendek D., Zagożdżon P. Selected dietary factors and breast cancer risk. Przegl Epidemiol. 2019; 73(3): 361–368, doi: 10.32394/pe.73.29.
12.
Abo Al-Shiekh S.S., Ibrahim M.A., Alajerami Y.S. Breast cancer knowledge and practice of breast self-examination among female university students, Gaza. ScientificWorldJournal 2021; 2021: 6640324, doi: 10.1155/2021/6640324.
13.
Koc G., Gulen-Savas H., Ergol S., Yildirim-Cetinkaya M., Aydin N. Female university students’ knowledge and practice of breast self-examination in Turkey. Niger J. Clin. Pract. 2019; 22(3): 410–415, doi: 10.4103/njcp.njcp_341_18.
14.
Heena H., Durrani S., Riaz M., AlFayyad I., Tabasim R., Parvez G. i wsp. Knowledge, attitudes, and practices related to breast cancer screening among female health care professionals: a cross sectional study. BMC Womens Health 2019; 19(1): 122, doi: 10.1186/s12905-019-0819-x.
15.
Reményi Kissné D., Gede N., Szakács Z., Kiss I. Breast cancer screening knowledge among Hungarian women: a cross-sectional study. BMC Womens Health 2021; 21(1): 69, doi: 10.1186/s12905-021-01204-9.
16.
Huq M.R., Woodard N., Okwara L., McCarthy S., Knott C.L. Breast cancer knowledge & information seeking among African American women below screening age. Patient Educ. Couns. 2023; 106: 194–200, doi: 10.1016/j.pec.2022.10.002.
17.
Nagórska M., Aksamit M., Krygowska K., Bassara-Nowak D. Determinants of women’s behavior in breast cancer prevention. Eur. J. Clin. Exp. Med. 2019; 17(2): 123–130, doi: 10.15584/ejcem.2019.2.3.
18.
Program profilaktyki raka piersi (mammografia). Ministerstwo Zdrowia – Portal Gov.pl [online] https://www.gov.pl/web/zdrowie...- [dostęp: 08.03.2024].
19.
Programy profilaktyczne. Narodowy Fundusz Zdrowia – NFZ [online] https://www.nfz.gov.pl/dla-pac... [dostęp: 08.03.2024].
20.
NBCF Team. Breast Self-Exam. National Breast Cancer Foundation [online], last updated on Jan 17, 2024, https://www.nationalbreastcanc... [dostęp: 08.03.2024].
21.
Kozierkiewicz A., Topór-Mądry R., Śliwczyński A., Pakulski M., Jassem J. Skuteczność i koszty leczenia raka piersi w Polsce; podejście regionalne. NOWOTWORY J. Oncol. 2014; 64(1): 24–32, doi: 10.5603/NJO.2014.0004.
22.
Paździor A., Stachowska M., Zielińska A. Wiedza kobiet na temat profilaktyki raka piersi. Nowiny Lek. 2011; 80(6): 419–422.
Share
RELATED ARTICLE
The Medical University of Silesia in Katowice, as the Operator of the annales.sum.edu.pl website, processes personal data collected when visiting the website. The function of obtaining information about Users and their behavior is carried out by voluntarily entered information in forms, saving cookies in end devices, as well as by collecting web server logs, which are in the possession of the website Operator. Data, including cookies, are used to provide services in accordance with the Privacy policy.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.