Current issue
Accepted manuscript
About the Journal
Scientific Council
Editorial Board
Regulatory and archival policy
Code of publishing ethics
Publisher
Information about the processing of personal data in relation to cookies and newsletter subscription
Archive
For Authors
For Reviewers
Contact
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Links
Sklep Wydawnictwa SUM
Biblioteka Główna SUM
Śląski Uniwersytet Medyczny w Katowicach
Privacy policy
Accessibility statement
Reviewers
Annals reviewers in 2025
Annals reviewers in 2024
Annals reviewers in 2023
Annals reviewers in 2022
Annals reviewers in 2021
Annals reviewers in 2020
Annals reviewers in 2019
Annals reviewers in 2018
Annals reviewers in 2017
Annals reviewers in 2016
Annals reviewers in 2015
Annals reviewers in 2014
Annals reviewers in 2013
Annals reviewers in 2012
Quality of life after transcatheter edge-to-edge mitral valve repair – prospective observational cohort study
1
Department of Cardiology and Structural Heart Diseases, Medical University of Silesia, Katowice, Poland
2
Students' Scientific Society, Medical University of Silesia, Katowice, Poland
3
Department of Cardiology, Medical University of Silesia, Katowice, Poland
Corresponding author
KEYWORDS
TOPICS
ABSTRACT
Introduction:
In patients with heart failure (HF), left ventricular remodeling can lead to secondary mitral regurgitation (SMR), which exacerbates HF symptoms and reduces quality of life (QoL). Transcatheter edge-to-edge repair (TEER), an interventional therapy for patients with SMR and high surgical risk, allows effective reduction of mitral regurgitation, leading to improved survival and quality of life. However, data on QoL outcomes post-TEER in the Polish population remain limited.
Material and methods:
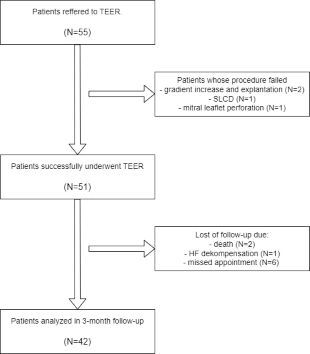
Aim of the study was to assess changes in QoL, measured by the Kansas City Cardiomyopathy Questionnaire (KCCQ-12), in patients with severe SMR undergoing TEER. This prospective, single-center, observational study included 42 consecutive patients with severe SMR who underwent TEER. Main outcome was QoL change after 3 months.
Results:
TEER was performed successfully in all cases without any major complications. An improvement in KCCQ-12 was observed in 38/42 (90.5%) of patients, mean KCCQ-12 score before and after 3-month was 41.9 ± 15.5 vs 61.4 ± 16.9, respectively (p < 0.001). The most significant improvement was observed among patients with lower initial QoL (r = -0.462; p = 0.002) and among patients without co-existing severe tricuspid regurgitation (Δ +21.7 vs +5.5; p = 0.04). During the follow-up period, only one patient required unplanned hospitalization.
Conclusions:
TEER is associated with a significant improvement in QoL at 3-month follow-up in patients with severe SMR. These findings support TEER as a valuable treatment strategy, providing important data for clinical practice in Poland.
In patients with heart failure (HF), left ventricular remodeling can lead to secondary mitral regurgitation (SMR), which exacerbates HF symptoms and reduces quality of life (QoL). Transcatheter edge-to-edge repair (TEER), an interventional therapy for patients with SMR and high surgical risk, allows effective reduction of mitral regurgitation, leading to improved survival and quality of life. However, data on QoL outcomes post-TEER in the Polish population remain limited.
Material and methods:
Aim of the study was to assess changes in QoL, measured by the Kansas City Cardiomyopathy Questionnaire (KCCQ-12), in patients with severe SMR undergoing TEER. This prospective, single-center, observational study included 42 consecutive patients with severe SMR who underwent TEER. Main outcome was QoL change after 3 months.
Results:
TEER was performed successfully in all cases without any major complications. An improvement in KCCQ-12 was observed in 38/42 (90.5%) of patients, mean KCCQ-12 score before and after 3-month was 41.9 ± 15.5 vs 61.4 ± 16.9, respectively (p < 0.001). The most significant improvement was observed among patients with lower initial QoL (r = -0.462; p = 0.002) and among patients without co-existing severe tricuspid regurgitation (Δ +21.7 vs +5.5; p = 0.04). During the follow-up period, only one patient required unplanned hospitalization.
Conclusions:
TEER is associated with a significant improvement in QoL at 3-month follow-up in patients with severe SMR. These findings support TEER as a valuable treatment strategy, providing important data for clinical practice in Poland.
REFERENCES (18)
1.
Huang AL, Dal-Bianco JP, Levine RA, Hung JW. Secondary Mitral Regurgitation: Cardiac Remodeling, Diagnosis, and Management. Struct Heart. 2022;7(3):100129. doi: 10.1016/j.shj.2022.100129.
2.
Wojakowski W, Chmielak Z, Widenka K, Pręgowski J, Perek B, Gackowski A, et al. Transcatheter mitral valve repair and replacement. Expert consensus statement of the Polish Cardiac Society and the Polish Society of Cardiothoracic Surgeons. Kardiol Pol. 2021;79(10):1165–1177. doi: 10.33963/KP.a2021.0116.
3.
Feldman T, Kar S, Elmariah S, Smart SC, Trento A, Siegel RJ, et al. Randomized Comparison of Percutaneous Repair and Surgery for Mitral Regurgitation: 5-Year Results of EVEREST II. J Am Coll Cardiol. 2015;66(25):2844–2854. doi: 10.1016/j.jacc.2015.10.018.
4.
Stone GW, Lindenfeld J, Abraham WT, Kar S, Lim DS, Mishell JM, et al. Transcatheter Mitral-Valve Repair in Patients with Heart Failure. N Engl J Med. 2018;379(24):2307–2318. doi: 10.1056/nejmoa1806640.
5.
Devlin NJ, Drummond MF, Mullins CD. Quality-Adjusted Life Years, Quality-Adjusted Life-Year-Like Measures, or Neither? The Debate Continues. Value Health. 2024;27(6):689–691. doi: 10.1016/j.jval.2024.04.021.
6.
Phyo AZZ, Freak-Poli R, Craig H, Gasevic D, Stocks NP, Gonzalez-Chica DA, et al. Quality of life and mortality in the general population: a systematic review and meta-analysis. BMC Public Health. 2020;20(1):1596. doi: 10.1186/s12889-020-09639-9.
7.
Spertus JA, Jones PG. Development and Validation of a Short Version of the Kansas City Cardiomyopathy Questionnaire. Circ Cardiovasc Qual Outcomes. 2015;8(5):469–476. doi: 10.1161/CIRCOUTCOMES.115.001958.
8.
Hausleiter J, Stocker TJ, Adamo M, Karam N, Swaans MJ, Praz F. Mitral valve transcatheter edge-to-edge repair. EuroIntervention. 2023;18(12):957–976. doi: 10.4244/EIJ-D-22-00725.
9.
Płońska-Gościniak E, Piotrowski G, Wojakowski W, Gościniak P, Olszowska M, Lesiak M, et al. Management of valvular heart disease in patients with cancer: Multidisciplinary team, cancer-therapy related cardiotoxicity, diagnosis, transcatheter intervention, and cardiac surgery. Expert opinion of the Association on Valvular Heart Disease, Association of Cardiovascular Interventions, and Working Group on Cardiac Surgery of the Polish Cardiac Society. Kardiol Pol. 2023;81(1):82–101. doi: 10.33963/KP.a2023.0023.
10.
Siudak Z, Grygier M, Tomaniak M, Kałużna-Oleksy M, Kleczyński P, Milewski K, et al. Interventional cardiology in Poland in 2023. Annual summary report of the Association of Cardiovascular Interventions of the Polish Cardiac Society (AISN PTK) and Jagiellonian University Medical College. Postepy Kardiol Interwencyjnej. 2024;20(4):379–381. doi: 10.5114/aic.2024.144970.
11.
Layoun H, Harb SC, Krishnaswamy A, Miyasaka R, Yun J, Kapadia SR. Patient Selection for Mitral Transcatheter Edge-to-Edge Repair. Methodist Debakey Cardiovasc J. 2023;19(3):26–36. doi: 10.14797/mdcvj.1199.
12.
Adamo M, Fiorelli F, Melica B, D’Ortona R, Lupi L, Giannini C, et al. COAPT-Like Profile Predicts Long-Term Outcomes in Patients With Secondary Mitral Regurgitation Undergoing MitraClip Implantation. JACC Cardiovasc Interv. 2021;14(1):15–25. doi: 10.1016/j.jcin.2020.09.050.
13.
Goel K, Lindenfeld J, Makkar R, Naik H, Atmakuri S, Mahoney P, et al. Transcatheter Edge-to-Edge Repair in 5,000 Patients With Secondary Mitral Regurgitation: COAPT Post-Approval Study. J Am Coll Cardiol. 2023;82(13):1281–1297. doi: 10.1016/j.jacc.2023.07.015.
14.
Lindman BR, Asch FM, Grayburn PA, Mack MJ, Bax JJ, Gonzales H, et al. Ventricular Remodeling and Outcomes After Mitral Transcatheter Edge-to-Edge Repair in Heart Failure: The COAPT Trial. JACC Cardiovasc Interv. 2023;16(10):1160–1172. doi: 10.1016/j.jcin.2023.02.031.
15.
Marut B, Istratoaie S, Leurent G, L’Official G, Auffret V, Oger E, et al. Reverse remodeling according to the aetiology after mitral TEER. Arch Cardiovasc Dis. 2025;118(1):S60. doi: 10.1016/j.acvd.2024.10.109.
16.
Brooks CJ, Duggal N, Seth M, Joseph MS, Sukul D, Chetcuti SJ, et al. Quality of Life After Mitral Transcatheter Edge-to-Edge Repair According to Baseline Tricuspid Regurgitation. Struct Heart. 2025;9(6):100408. doi: 10.1016/j.shj.2024.100408.
17.
Agrawal A, Ramu SK, Shekhar S, Isogai T, Bansal A, Yun J, et al. Impact of Noncardiac Co-Morbidities in Patients Who Underwent Transcatheter Edge-to-Edge Mitral Valve Repair on Outcomes. Am J Cardiol. 2023;204:401–404. doi: 10.1016/j.amjcard.2023.07.078.
18.
Reddy YNV, Rikhi A, Obokata M, Shah SJ, Lewis GD, AbouEzzedine OF, et al. Quality of life in heart failure with preserved ejection fraction: importance of obesity, functional capacity, and physical inactivity. Eur J Heart Fail. 2020;22(6):1009–1018. doi: 10.1002/ejhf.1788.
Share
RELATED ARTICLE
The Medical University of Silesia in Katowice, as the Operator of the annales.sum.edu.pl website, processes personal data collected when visiting the website. The function of obtaining information about Users and their behavior is carried out by voluntarily entered information in forms, saving cookies in end devices, as well as by collecting web server logs, which are in the possession of the website Operator. Data, including cookies, are used to provide services in accordance with the Privacy policy.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.
You can consent to the processing of data for these purposes, refuse consent or access more detailed information.